|
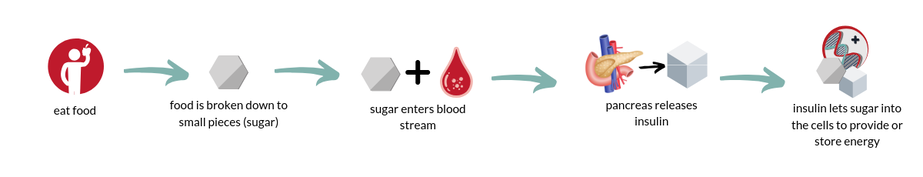
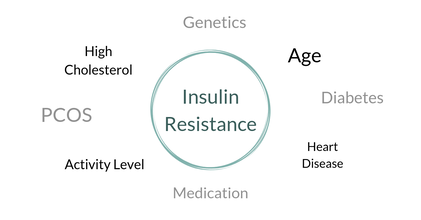
Many of you have heard the term insulin resistance, probably from a doctor in relation to a health condition. However, a lot of times health care providers forget that words like insulin resistance don’t mean anything to people outside of the healthcare sector. To understand insulin resistance, you have to know what insulin is AND how the body uses insulin to regulate biologic processes AND how that could impact your specific condition. Throughout this post we will work through what insulin resistance is and how it may be impacting your health. Let’s start at the very beginning. When you eat food, it gets broken down to provide your body with energy. Carbohydrates (basically any thing that started out as a plant, bread, pasta, rice, fruit, veggies, sugar, etc.) get broken down into sugar (or glucose if we are being fancy). Sugar is the fuel source our cells prefer to use. Think of it like your car, there are three basic types of fuel, gasoline, diesel, and electric. You have a regular car and it prefers standard gasoline, glucose is the gasoline of the body. So sugar enters the bloodstream for our cells to use as energy. But for our cells to be able to use the sugar, INSULIN is needed to let the sugar in. WHAT IS INSULIN? Insulin is made in your pancreas. Insulin is a hormone. A hormone is a signal in the body that tells it to do something. In this case, insulin is most famous for telling the various cells in the body take sugar out of your blood. But here’s a fun fact, insulin is also needed for your muscles to use protein, but not as much is needed to use protein compared to carbs. This is why the ketogenic diet is often recommended to people who have conditions derived from insulin resistance (PCOS, diabetes, etc.) because fat doesn’t require ANY insulin to be released. So when you eat, protein and carbs, they signal your pancreas to release insulin, and insulin tells your body to use the protein and carbs. Insulin is what we call anabolic, or a hormone that likes to store energy. This means that when there is excess carbohydrate in the blood, insulin would like to store it for later. When your cells pick up the sugar in your blood, they either use it immediately for energy or they store it in your muscle or fat for later if you don’t need it right away. This also means that your body uses insulin more efficiently (pulls more sugar out of the blood) when your cells need energy the most, say during/after exercising because you either need energy now or you need to replenish the energy stores you used up.
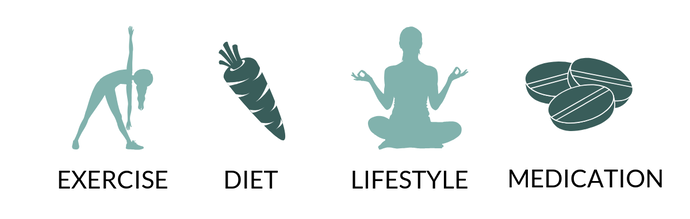
HOW DO I KNOW IF I HAVE INSULIN RESISTANCE? The best way to know if you have insulin resistance is to get you blood work done. Typically you’ll want to get an A1c checked, this indicates your average blood sugar levels over the last three months, a fasting glucose level to see what your body is doing right now, an insulin level to see if you’re producing a normal amount of the hormone, and a C-peptide level which helps interpret your insulin level. Without getting labs done, there is no way to know for sure if you have insulin resistance. However, if you have darkened skin (compared to the rest of your body) on the back of your neck or around your armpit region you might have insulin resistance. HOW DO I IMPROVE INSULIN SENSITIVITY? The biggest question here is “If I have insulin resistance, what do I do about it?” Since insulin resistance is so individualized, you really should talk to someone (preferably a healthcare provider) who specializes in managing insulin resistance. When looking for this person, I would recommend avoiding anyone who gives you a cut and dry answer, because you really need someone who will assess what is right for your preferences and your lifestyle and walk you through how you can implement that in your own life. Overall there are four avenues you can explore for managing insulin resistance; diet, exercise, lifestyle, and medication. Exercise: As we talked about earlier, exercise makes your cells more insulin sensitive because they either need energy or need to replace spent energy. If exercise isn’t your thing it can really be boiled down to movement. After you eat, specifically in the hour after you eat when blood sugars will be the highest, go for a short walk (at least 10 minutes), stay standing and do some chores, or literally anything else that involves moving your body. Diet: Okay, this one is a little controversial and one of the main reasons you should find someone who can help you find the right path for you (*cough* a dietitian *cough*). I mentioned the ketogenic diet earlier and that’s an option, the focus on fat as energy reduces the insulin secreted in the first place, BUT you still need to EAT YOUR VEGGIES (that’s a whole other conversation, but please!). Intermittent Fasting (IF) is another option. IF helps reduce insulin because when you eat in a time restricted window your pancreas isn’t kicking out insulin all day to process the food you’ve been eating. You could focus on counting carbohydrate or eating more carbohydrates that have less of an impact on insulin levels. Or you could always try Intuitive Eating which tells you to eat what you want when you want to and although it may be a longer process than the other two options, you’ll probably end up happier and less stressed about food. There are some other strategies as well but I’m just going to defer to having you ask someone who can walk you through what best best choice is for you based on your labs and your lifestyle. Lifestyle: Lifestyle is another huge impact on insulin resistance. Major players: poor sleep, high stress, and injuries causing inflammation (that’s another topic as well). Each of these things, plus other factors that cause inflammation will decrease your insulin sensitivity. If you think that lack of sleep and high stress are really prevalent in your life, you might start your journey here. Medication: You can always turn to medication to help manage your insulin resistance. Ask your doctor what they recommend to help you start managing blood sugar levels. You can/should still work on the other avenues of managing insulin resistance, but medication can provide you with immediate relief and can help reduce your risk for conditions associated with insulin resistance while you work on your lifestyle, diet, and/or exercise. Insulin resistance is tricky, but if you’re interested in managing an associated condition or reducing risk for a condition, you have treatment options!
Let me know in the comments you this post was helpful and improved your understanding of insulin resistance. REFERENCES https://www.everydayhealth.com/type-2-diabetes/insulin-resistance-causes-symptoms-diagnosis-consequences/ https://www.nih.gov/news-events/news-releases/nih-study-shows-how-insulin-stimulates-fat-cells-take-glucose https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3277302/ https://www.verywellhealth.com/pcos-and-insulin-resistance-2616319#the-connection https://www.ncbi.nlm.nih.gov/pmc/articles/PMC380258/pdf/JCI0010842.pdf https://emedicine.medscape.com/article/2089224-overview#a2 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5336429/#!po=15.0000
1 Comment
12/4/2019 05:22:32 am
Living a sedentary lifestyle is solely responsible for many health-related disorders.
Reply
Leave a Reply. |